What Is Pancreatic Cancer? Causes, Symptoms, and Treatment Options
Pancreatic cancer is a disease that begins when abnormal cells in the pancreas, an organ located behind the stomach, grow out of control and form a tumor. This type of cancer is particularly challenging because it often does not show symptoms in its early stages, making early detection difficult. The pancreas plays a vital role in your body by producing enzymes that help with digestion and hormones like insulin that control your body’s blood sugar levels. When a tumor develops, it can interfere with these crucial functions and spread to other parts of the body. Understanding the causes, recognizing the symptoms, and exploring treatment options are critical steps in managing this condition.
Chat with us on WhatsApp (Free): +90 530 917 30 30
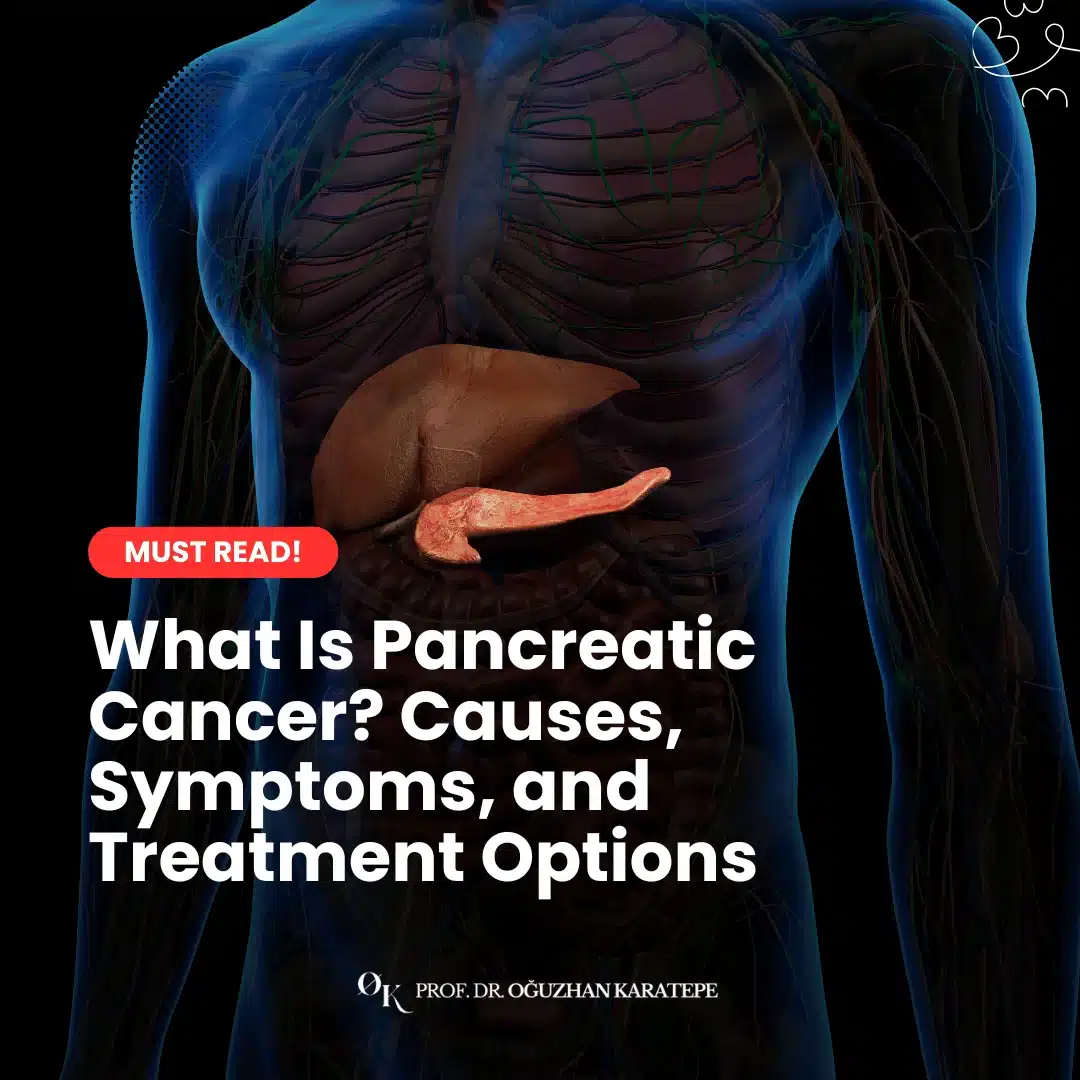
Understanding the Pancreas and Its Function
Before diving into the specifics of pancreatic cancer, it’s helpful to understand what the pancreas does. The pancreas is a gland about six inches long, shaped like a flat pear, and situated in the abdomen, tucked behind the stomach. It has two main jobs in the body:
- Exocrine Function: The pancreas produces powerful enzymes that help break down fats, proteins, and carbohydrates in the small intestine. These enzymes travel from the pancreas to the small intestine through a system of ducts.
- Endocrine Function: The pancreas also creates important hormones, most notably insulin and glucagon. These hormones are released directly into the bloodstream and work together to manage the body’s blood sugar levels. Insulin helps cells use sugar for energy, while glucagon raises blood sugar when it’s too low.
Cancer can develop in either the exocrine or endocrine cells of the pancreas, but over 95% of pancreatic cancers are exocrine tumors, known as pancreatic ductal adenocarcinoma. These start in the cells lining the ducts that carry digestive enzymes.
What Causes Pancreatic Cancer?
The exact cause of pancreatic cancer is not fully understood, but researchers have identified several risk factors that increase the likelihood of developing the disease. It occurs when the DNA of pancreatic cells undergoes changes (mutations) that cause them to multiply uncontrollably and form a mass, or tumor. While some of these mutations are inherited, most happen for reasons that are not yet known.
Major Risk Factors for Pancreatic Cancer
While having one or more risk factors doesn’t mean you will definitely get pancreatic cancer, they do increase your chances. Key risk factors include:
- Smoking: This is one of the most significant and preventable risk factors. Smokers are about twice as likely to develop pancreatic cancer as non-smokers.
- Age: The risk increases significantly with age. The vast majority of cases occur in people over the age of 60.
- Family History and Genetics: If your mother, father, or sibling had pancreatic cancer, your risk is higher. Certain genetic syndromes can also increase the risk.
- Chronic Pancreatitis: Long-term inflammation of the pancreas is a strong risk factor.
- Sugar Disease (Diabetes): People with long-standing sugar disease, particularly Type 2, have an increased risk. Conversely, the sudden onset of sugar disease in an older adult can sometimes be an early symptom of pancreatic cancer.
- Obesity: Being significantly overweight increases the risk of developing this cancer.
- Diet: A diet high in red and processed meats and low in fruits and vegetables may increase the risk.
Can Pancreatic Cancer Be Prevented?
While there is no guaranteed way to prevent pancreatic cancer, you can take steps to lower your risk. The most effective step is to stop smoking. Maintaining a healthy weight through a balanced diet and regular physical activity is also crucial. Limiting alcohol consumption can help prevent pancreatitis, which in turn reduces your cancer risk.
Chat with us on WhatsApp (Free): +90 530 917 30 30
What Are the Early Symptoms of Pancreatic Cancer?
Early symptoms of pancreatic cancer can be vague and easy to ignore, which is why the disease is often diagnosed at a later stage. The symptoms largely depend on the location of the tumor within the pancreas. As the tumor grows, it can press on nearby organs and nerves, leading to more noticeable signs.
Common Signs and Symptoms to Watch For
If you experience any of the following symptoms persistently, it is important to consult a healthcare professional for a proper evaluation.
- Jaundice (Yellowing of the Skin and Eyes): This is one of the most common symptoms, especially if the tumor is in the head of the pancreas. The tumor can block the bile duct, causing a buildup of bilirubin in the body. This can also lead to dark urine, pale stools, and itchy skin.
- Abdominal or Back Pain: A dull ache or pain in the upper abdomen that may radiate to the back is common. The pain can become more persistent as the tumor grows and presses on surrounding nerves.
- Unexplained Weight Loss and Loss of Appetite: Losing weight without trying is a frequent and concerning sign. This can be coupled with a feeling of fullness after eating very little.
- Changes in Stool: Stools may become pale, greasy, and float (a condition called steatorrhea) because the tumor is blocking the flow of pancreatic enzymes needed to digest fat.
- New-Onset Sugar Disease: The sudden development of sugar disease in an individual over 50, especially without a family history or weight gain, can be an early warning sign.
- Nausea and Vomiting: If the tumor presses on the stomach, it can make you feel sick and lead to vomiting.
- Blood Clots: In some cases, the first sign of pancreatic cancer can be a blood clot in a large vein, often in the leg (deep vein thrombosis or DVT).
When Should You See a Doctor?
It is crucial to see a doctor if you have persistent symptoms like unexplained weight loss, jaundice, or abdominal pain. While these can be caused by many other conditions, getting an accurate diagnosis as soon as possible is essential for effective management and treatment.
Chat with us on WhatsApp (Free): +90 530 917 30 30
How Is Pancreatic Cancer Diagnosed?
Diagnosing pancreatic cancer involves a combination of a physical examination, a review of your medical history, imaging tests, and sometimes a tissue sample. Because the pancreas is located deep within the body, a physical exam alone is often not enough to detect a small, early-stage tumor.
Diagnostic Tests and Procedures
If your doctor suspects pancreatic cancer, they may recommend several tests to confirm the diagnosis and determine the extent (stage) of the cancer.
- Imaging Tests: These create detailed pictures of your pancreas and surrounding organs.
- CT (Computed Tomography) Scan: This is often the first imaging test used. It provides detailed cross-sectional images that can show a tumor in the pancreas.
- MRI (Magnetic Resonance Imaging): An MRI can provide more detailed images and is particularly useful for examining the bile and pancreatic ducts.
- PET (Positron Emission Tomography) Scan: This scan can help determine if the cancer has spread to other parts of the body (metastasized).
- Endoscopic Ultrasound (EUS): A thin, flexible tube with a small camera and ultrasound probe is passed through your mouth and into your small intestine. This allows the doctor to get very close to the pancreas for detailed images and to take a tissue sample (biopsy).
- Biopsy: The only way to be certain of a pancreatic cancer diagnosis is to examine a small piece of the tumor tissue under a microscope. This is most commonly done during an EUS.
- Blood Tests: Doctors may check for tumor markers, such as CA 19-9. High levels of CA 19-9 can be a sign of pancreatic cancer, but this test is not used for screening as other conditions can also raise these levels. It is more often used to monitor treatment response.
Understanding the Stages of Pancreatic Cancer
Staging is the process of determining how much cancer is in the body and where it has spread. This information is crucial for planning the most effective treatment. The stage is determined by the size of the tumor, whether it has spread to nearby lymph nodes, and whether it has spread to distant organs like the liver or lungs.
- Stage 0 (Resectable): The cancer is confined to the top layers of pancreatic duct cells and has not spread. It is surgically removable.
- Stage I (Resectable): The tumor is still confined to the pancreas and is small enough to be surgically removed.
- Stage II (Resectable/Borderline Resectable): The tumor may have grown outside the pancreas or into nearby lymph nodes but has not spread to major blood vessels. Surgery may still be an option.
- Stage III (Locally Advanced/Unresectable): The cancer has spread to major nearby blood vessels or nerves, making it impossible to remove completely with surgery.
- Stage IV (Metastatic): The cancer has spread to distant organs, such as the liver, lungs, or abdominal cavity.
What Are the Treatment Options for Pancreatic Cancer?
Treatment for pancreatic cancer depends heavily on the stage of the cancer, your overall health, and your personal preferences. A team of specialists, including a surgeon, a medical oncologist, and a radiation oncologist, will work together to create a personalized treatment plan. The main goals of treatment are to remove the cancer if possible, stop it from spreading, and relieve symptoms to improve quality of life.
Chat with us on WhatsApp (Free): +90 530 917 30 30
Surgery for Pancreatic Cancer
Surgery offers the best chance for long-term control of pancreatic cancer, but it is only an option if the cancer has not spread to distant sites and can be completely removed. The type of surgery depends on the tumor’s location.
- Whipple Procedure (Pancreaticoduodenectomy): This is the most common surgery for tumors in the head of the pancreas. It is a complex operation where the surgeon removes the head of the pancreas, the gallbladder, part of the small intestine, and part of the bile duct.
- Distal Pancreatectomy: This procedure is used for tumors in the body or tail of the pancreas. The surgeon removes the tail and body of the pancreas, and often the spleen as well.
- Total Pancreatectomy: In rare cases, the entire pancreas is removed. Patients will need to take insulin and pancreatic enzyme supplements for the rest of their lives.
Chemotherapy
Chemotherapy uses powerful drugs to kill cancer cells throughout the body. It can be given before surgery (neoadjuvant) to shrink the tumor, after surgery (adjuvant) to kill any remaining cancer cells, or as the main treatment for advanced cancer that has spread.
Radiation Therapy
Radiation therapy uses high-energy beams, such as X-rays, to destroy cancer cells. It is often used in combination with chemotherapy, either before surgery to shrink the tumor or to treat locally advanced cancers that cannot be removed surgically. It can also be used to relieve symptoms like pain.
Targeted Therapy and Immunotherapy
These are newer forms of treatment. Targeted therapy drugs focus on specific abnormalities within cancer cells. Immunotherapy works by helping your body’s own immune system recognize and fight the cancer. These treatments are typically used for specific types of pancreatic cancer or in cases where other treatments are no longer working.
What is the Recovery Process After Pancreatic Cancer Surgery?
Recovery from pancreatic cancer surgery is a significant process that requires patience and careful management. A hospital stay of one to two weeks is typical. During this time, the medical team will manage pain, monitor for complications, and slowly reintroduce food. After returning home, recovery continues for several weeks or months. You will need to follow a special diet and may need to take pancreatic enzyme supplements to help with digestion. Regular follow-up appointments are essential to monitor your recovery and check for any signs of the cancer returning.
Why Choose Prof. Dr. Oğuzhan Karatepe for Pancreatic Cancer Treatment?
Navigating a pancreatic cancer diagnosis requires a team with profound expertise and experience. Prof. Dr. Oğuzhan Karatepe is a leading general surgeon with over 25 years of dedicated experience in complex oncological surgeries. Having performed more than 3,000 surgeries and contributed hundreds of articles to national and international medical literature, his expertise in pancreatic, liver, and gastrointestinal cancers is well-established. Prof. Dr. Karatepe is recognized as one of Turkey’s top doctors in his field, bringing a high level of surgical skill and a deep understanding of cancer care to each patient. Our team is committed to providing professional, comprehensive care tailored to your individual needs.
Chat with us on WhatsApp (Free): +90 530 917 30 30
How to choose the best pancreatic cancer doctor?
Choosing the right doctor is a critical decision. Look for a surgeon who specializes in pancreatic surgery, often referred to as a hepato-pancreato-biliary (HPB) surgeon. High-volume surgeons and hospitals—those that perform many of these complex operations—tend to have better outcomes. It’s also important to find a doctor who works with a multidisciplinary team and who communicates clearly and compassionately, ensuring you are a partner in your own care.
Which doctor treats the pancreas?
The treatment of pancreatic cancer is a team effort. A General Surgeon or a specialized HPB (Hepato-Pancreato-Biliary) Surgeon performs the surgery. A Medical Oncologist manages chemotherapy and other drug-based treatments. A Radiation Oncologist oversees radiation therapy. Your care will be coordinated among these and other specialists, such as gastroenterologists and dietitians.
Frequently Asked Questions (FAQ)
How long can you live with pancreatic cancer?
Prognosis varies greatly depending on the stage at diagnosis, the patient’s overall health, and the treatment response. For early-stage, localized cancer that can be surgically removed, the outlook is more favorable. For advanced-stage cancer, the focus of treatment is often on extending life and managing symptoms. It is important to discuss your specific situation with your medical team.
Is pancreatic cancer surgery a major operation?
Yes, surgeries for pancreatic cancer, like the Whipple procedure, are among the most complex and demanding abdominal operations. They require a highly skilled surgical team and a comprehensive post-operative care plan.
What is the Whipple procedure success rate?
The success of the Whipple procedure is measured both by the surgeon’s ability to safely perform the operation with minimal complications and by its effectiveness in controlling the cancer. In major medical centers with experienced surgeons, the immediate safety of the procedure is very high. Long-term success depends on the stage of the cancer at the time of surgery.
Can you live a normal life without a pancreas?
Yes, it is possible to live without a pancreas, but it requires lifelong medical management. You would need to take insulin injections to control blood sugar (as you would have surgically-induced sugar disease) and take enzyme replacement pills with every meal to digest food properly.
What is the difference between pancreatic cancer and pancreatitis?
Pancreatitis is the inflammation of the pancreas, which can be acute (sudden) or chronic (long-lasting). It is not cancer. However, chronic pancreatitis is a significant risk factor for developing pancreatic cancer.
Is pancreatic cancer genetic?
About 10% of pancreatic cancers are thought to have a genetic component, meaning they run in families. If you have two or more first-degree relatives who have had pancreatic cancer, your risk is higher, and you may wish to discuss genetic counseling with your doctor.
What are the survival rates for pancreatic cancer by stage?
Survival rates are statistics that provide a general idea of the outlook. For localized pancreatic cancer, the five-year survival rate is significantly higher than for cancer that has spread to distant parts of the body. These numbers are averages and cannot predict an individual’s outcome.
What should I eat after pancreatic cancer surgery?
After surgery, your digestive system will need time to heal. You will likely start with clear liquids and gradually move to solid foods. A diet of small, frequent, low-fat meals is often recommended. A dietitian will provide specific guidance, and you may need to take pancreatic enzyme supplements.
How painful is pancreatic cancer?
Pain is a common symptom, particularly as the tumor grows and presses on nerves. However, pain can be effectively managed. Pain management is a key part of the overall treatment plan and can involve medications, radiation therapy, or nerve blocks.
Does sugar feed pancreatic cancer?
All cells in the body, including cancer cells, use sugar (glucose) for energy. However, there is no conclusive scientific evidence that eating a sugar-free diet will stop pancreatic cancer from growing. A balanced, nutritious diet is most important for maintaining strength during treatment.
Contact Us Now
Facing a diagnosis of pancreatic cancer can be overwhelming. Having an experienced and dedicated medical team by your side is essential. Our expert team, led by Prof. Dr. Oğuzhan Karatepe, is ready to provide professional support and guidance for the surgical treatment of pancreatic cancer. We are here professionally for you.
Chat with us on WhatsApp (Free): +90 530 917 30 30
How can I book an appointment?
You can reach our team to schedule a consultation by contacting us via phone, WhatsApp, or through the online appointment form on our website. We are ready to assist you.
Legal Disclaimer
Attention: This information is for general knowledge only. It is not a substitute for professional medical advice, diagnosis, or treatment. For personalized treatment and medical guidance, please contact us to consult with a qualified healthcare professional.

